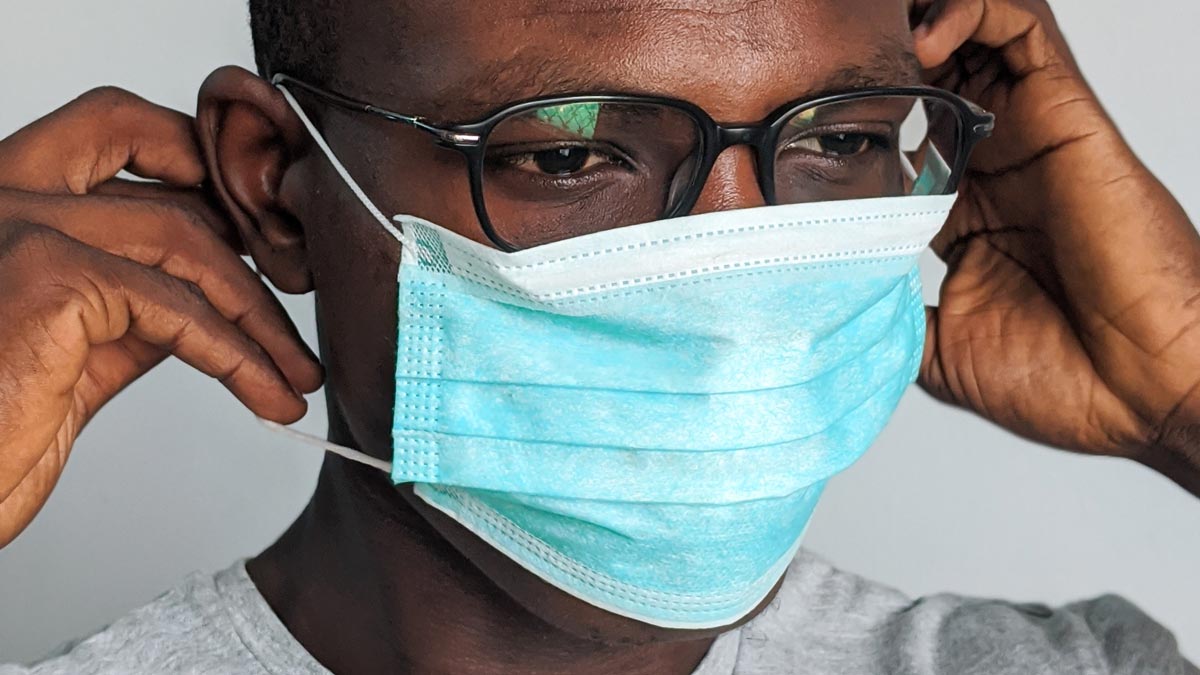
When you’re stuck in neurodivergent survival mode
Let me ask you something that rarely gets asked: Where in your body do you hold your mask?
Is it in your jaw, clenched tight from too many polite smiles? In your chest, where the tension builds every time you pretend to be calm when you’re anything but?
In your gut, coiled and uneasy from constantly overanalyzing what you just said, how you said it, and whether it came across “normal” enough?
For many neurodivergent people, masking is something our nervous systems learn to do. Constantly. Until it becomes a default state. Until it becomes our baseline.
This is what I call neurodivergent survival mode. A state where we’re fighting to exist in environments that feel unsafe in subtle, persistent ways.
And most of the time? We don’t even realize we’re doing it. We just know we’re tired, anxious, burnt out, or shutting down.
Masking Is a Nervous System Strategy
When people talk about masking, they usually focus on the outward signs: making eye contact even when it feels unnatural, managing your tone to sound “friendly” enough, suppressing stims like hand-flapping or rocking, forcing yourself through small talk to avoid seeming “rude.”
But masking is far more than social performance. It’s not just about what you do, but rather about what your nervous system has learned to expect. And fear.
For neurodivergent people, masking is a survival response. It starts early, often after the first time someone tells you to “stop being weird,” “calm down,” or “act normal.” That moment doesn’t just register in your mind.
Masking Lives in the Body: Understanding Neurodivergent Survival Mode
When people talk about masking, they often picture something mental or behavioral: memorizing scripts, forcing eye contact, mimicking social norms, smiling when it hurts.
But for neurodivergent people, masking is a physiological adaptation. It’s your body doing whatever it must to keep you “safe” in a world that punishes difference.
The first time you were corrected for your tone. Or laughed at for a meltdown. Or told you were too much, too intense, too emotional. That moment taught your nervous system a rule: “Being myself isn’t safe.” And once that lesson sinks in, your body doesn’t wait for logic. It responds to perceived threat on autopilot.
This is neurodivergent survival mode. And it shows up in one of four primary responses your nervous system initiates without conscious thought:
- Fight: You feel irritated or defensive. You argue, interrupt, over-explain.
- Flight: You shut down. You ghost, log off, or mentally check out. You leave before you can be left.
- Freeze: You go still. Your brain fogs. Speech vanishes. You might nod along, but you can’t access language or action.
- Fawn: You get extra nice. You smile when you want to cry. You agree even when it hurts. You over-function, over-apologize, over-accommodate, because pleasing feels safer than being seen.
These responses become daily rituals for many neurodivergent folks. We live in systems where misunderstanding, overstimulation, and invalidation are routine. Which means the “threat” our bodies are trying to navigate is social harm, sensory overload, or emotional dismissal.
So if you’re constantly contorting just to make others comfortable, your nervous system never really gets to relax. Even in “safe” spaces, you stay on edge. Even in silence, your body is bracing. Over time, this survival mode becomes background noise. Normal. Expected. Invisible.
Until something breaks. Or you do.
When Survival Mode Becomes a Lifestyle
For most people, fight-or-flight is a response to immediate danger. For example, a car swerves, a loud noise, a sudden confrontation. Many neurodivergents find themselves perpetually trapped int his state.
You might wake up already bracing, heart rate elevated before you’ve even had coffee. Or you might walk into a room scanning for tone, posture, and mood like your wellbeing depends on it.
You might go through a workday rehearsing every message, every sentence, every micro-expression, only to come home and collapse, unable to answer a simple “How was your day?”
This is the invisible reality of neurodivergent survival mode. And while it may have helped you survive certain environments (school, family, the workplace), long-term, it takes a toll.
Here’s what chronic survival mode can look like in the body:
- Digestive issues that flare under stress
- Tension headaches and jaw pain from clenching
- Fatigue that sleep doesn’t fix
- Trouble falling asleep, or waking up already exhausted
- Executive dysfunction that leaves you unable to start, plan, or follow through
- Sensory intolerance that intensifies the more burnt out you get
- Emotional volatility or total shutdowns over things that “shouldn’t” be a big deal
And here’s the cruel twist: the better you are at masking, the more likely you are to be overlooked, dismissed, or misread. Because you’re still smiling. Still meeting deadlines. Still saying “I’m fine.”
But underneath that mask? Your nervous system is in overdrive. Your body is screaming for rest, regulation, relief. And no one sees it. Maybe not even you.
When You Can’t Fake It Anymore
Maybe you’ve said things like: “I’m just tired all the time.” “I thought I was fine until I hit a wall.” “I don’t know why I can’t handle things like I used to.”
That wall you hit? It’s your nervous system waving a white flag, saying: “I can’t keep pretending. I need help.”
For neurodivergent people, this moment often comes without warning, or rather, without recognized warning. Because the signs were there all along, just buried beneath years of performance.
By the time burnout sets in, the symptoms are everywhere:
- Your memory starts to glitch. Names, dates, basic words go missing
- Your ability to initiate tasks evaporates, even for things you enjoy
- Conversations become draining, even with people you love
- Your fuse shortens, or disappears completely
- Rest no longer feels restful; nothing feels replenishing
These can all be signs of nervous system collapse. Your body is no longer running on stress hormones and adrenaline. It’s run out. And when it does, it stops letting you mask.
You might find yourself crying unexpectedly, snapping at small things, needing to cancel plans, or freezing mid-task. And suddenly, the coping strategies that used to “work” no longer do.
That’s the thing about neurodivergent survival mode: it doesn’t ask for permission to shut down. It just does. Because at some point, the mask gets too heavy. And your body decides: “Survival means stopping now.”
Unmasking Begins in the Body
When you’ve spent years masking—holding tension, bracing for rejection, filtering every word—it’s easy to think the fix must be cognitive. That you can journal or analyze your way out. That if you just understood yourself better, the burnout would lift.
You see, masking is both a habit of the mind and a pattern in the body.
Your jaw tightens before you speak. Your shoulders tense when someone walks in the room. You hold your breath during Zoom calls or group chats. You smile on autopilot, even when you’re crumbling inside.
These are data points; your body’s way of saying, “This feels unsafe.”
Unmasking begins when we read these data points and respond with compassion.
It might look like:
- Noticing when you say “yes” but feel “no” in your chest
- Allowing yourself to stim, rock, pace, fidget, without explanation
- Taking a break before your body demands one
- Feeling yourself breathe all the way down to your belly—for the first time in years
These small acts tell your nervous system: I’m listening now. I don’t need you to be on high alert all the time.
This is how you begin to exit neurodivergent survival mode: by reintroducing safety from the inside out.
By reclaiming the option to choose when, where, and how you show up.
What Safety Actually Feels Like
So what happens when the body begins to feel safe again? When masking isn’t your only survival strategy? When you’re no longer performing at every turn just to stay accepted?
Something subtle but profound starts to shift. You move from coping to connecting.
Because here’s what many neurodivergent people never get told: it’s nearly impossible to experience real connection, whether with yourself or others, when you’re in survival mode.
Survival narrows your field of vision. It makes every interaction feel like a potential threat. You scan for tone. You edit your reactions. You rehearse your lines. In short: you’re managing the risk of rejection.
But when your nervous system feels safe? When regulation becomes more familiar than vigilance?
Everything softens.
- You hear what someone’s saying instead of planning your next sentence
- You notice you’re overstimulated and step away before you shut down
- You ask for clarity instead of pretending to understand
- You receive care without guilt; offer care without depletion
- You say what you actually mean, not what you think they want to hear
This is where unmasking becomes relational, and you start experiencing safety while being yourself.
You stop filtering everything through the question, “Will this make me weird?” You stop bracing every time someone texts, “Can we talk?” You stop leaving conversations with a shame hangover and imaginary apologies.
And maybe—just maybe—you begin to feel liked for the version of you that’s honest. Present. Embodied. Enough.
That shift doesn’t happen overnight. It’s slow. Uneven. Sometimes scary. But it’s real.

We Heal in Safe Company
When you’ve spent your life being told you’re too much, too sensitive, too intense, it’s easy to assume that healing must be a solo project. You’ve learned to mask for safety, but also for acceptance. So unmasking can feel like a risk no one else should be responsible for.
But you didn’t learn to mask in isolation. You were taught—through subtle cues, outright punishments, and daily misunderstandings—that who you are is a problem to be fixed.
And so it makes sense that healing won’t happen in isolation either. In fact, it can’t.
To unlearn survival mode, we need evidence that the world is safer than it once was. And the nervous system doesn’t learn that through logic. It learns through felt experience, especially in relationships.
Maybe that looks like:
- A friend who lets you stim without comment
- A therapist who doesn’t rush your words, or pathologize your silence
- A partner who lets you take breaks mid-conversation without taking it personally
- A coworker who honors your need for clarity, or quiet, or processing time
- Even a pet who shares space with you, no questions asked
These moments may seem small, but to a nervous system that’s spent years in survival, they’re revolutionary. They say: “You don’t have to perform here.” “You’re not being judged.” “You can stay.”
And every time your body receives that message and nothing bad happens, it recalibrates. It learns. It heals.
This is the slow, sacred work of exiting neurodivergent survival mode. Not just through solitude or introspection, but through co-regulation; experiences of being safe with someone.
If that feels foreign, that’s okay. It means your nervous system hasn’t had enough practice with safety.
But you can begin now by seeking or creating even one space where the mask can loosen, where you can breathe, where you don’t have to explain why something hurts.
And maybe, in that space, your body will finally believe: You’re allowed to be here, exactly as you are.
Final Thoughts
You may have heard the phrase, “The body keeps the score.” It’s often used to describe how trauma lives on in the nervous system, and how the body remembers things the mind tries to forget.
But here’s something just as true: the body doesn’t just keep the score. It keeps the truth.
It knows when your smile is a shield. It knows when your “I’m fine” is a freeze response. It knows when you’re pushing through exhaustion because you don’t feel like you’re allowed to stop.
And maybe most importantly, it remembers who you were before the mask. Before you had to contort and filter and apologize just to be allowed to stay.
Even if you don’t remember that version of yourself. Even if it’s buried under decades of performance. Even if you’ve never known what it feels like to be fully, safely you, your body does.
So if you’re exhausted… If your fuse is short… If you feel like you’re unraveling for no clear reason…
Please hear this: your nervous system learned to protect you in the only ways it could. And now? It might be asking to try something new.
Not all at once. Not overnight. But slowly. Gently. Deliberately.
Because the body that carried your survival also holds the blueprint for your healing. And maybe—for the first time—it’s finally safe enough to listen.
Have you been stuck in neurodivergent survival mode? Where in your body do you feel it most? What helps you come back to yourself?

Essy Knopf is a therapist who likes to explore what it means to be neurodivergent and queer. Subscribe to get all new posts sent directly to your inbox.